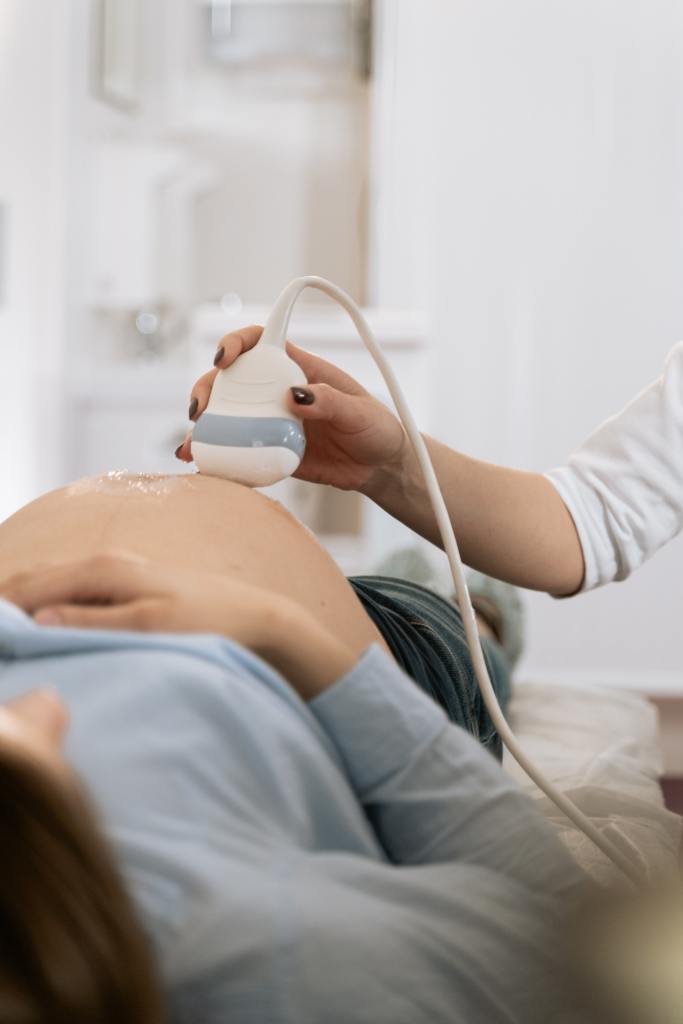
You’ll undergo many blood tests during your pregnancy. However, the pregnancy glucose test is a rite of passage.
Unlike previous bloodwork, this second-trimester test isn’t an in-and-out affair. Instead, this test requires you to have your blood drawn. Then, you’ll drink a sugary beverage that tastes like flat orange, lime, or berry soda. After waiting in the office for an hour, you’ll be called back for another blood draw.
The 1-hour glucose test when pregnant screens for gestational diabetes, which is diabetes that occurs in pregnant people who were not previously diabetic. It’s not fun, but it’s important. Gestational diabetes can pose risks to a developing baby and pregnant person if the condition isn’t monitored or managed.
So, you took the test to be safe and hoped to move on with your life, perhaps planning your baby shower cake design.
Then, you get a call from your OBGYN. You failed the 1-hour test. Now what?
Breathe. Here’s what happens next.

You might be able to take another test
If you didn’t pass your 1-hour pregnancy glucose test, it means your blood sugar levels were elevated enough to raise a flag.
However, the 1-hour test isn’t considered diagnostic. It’s a screen that casts a wide net to ensure doctors don’t miss anyone with gestational diabetes.
According to the CDC, 2% to 10% of pregnant people develop gestational diabetes yearly. It’s unclear how many people fail the 1-hour glucose test when pregnant, but most who do will not have gestational diabetes.
If your blood sugar levels exceed 140, your physician might ask you to take a longer test. This test requires fasting, and you’ll have your blood drawn three or four times (once before you consume the beverage and two or three times after — the post-drink draws will happen 1 hour and 2 hours after, and possibly 3 hours after). If your numbers are in check, you won’t be diagnosed with gestational diabetes — phew.
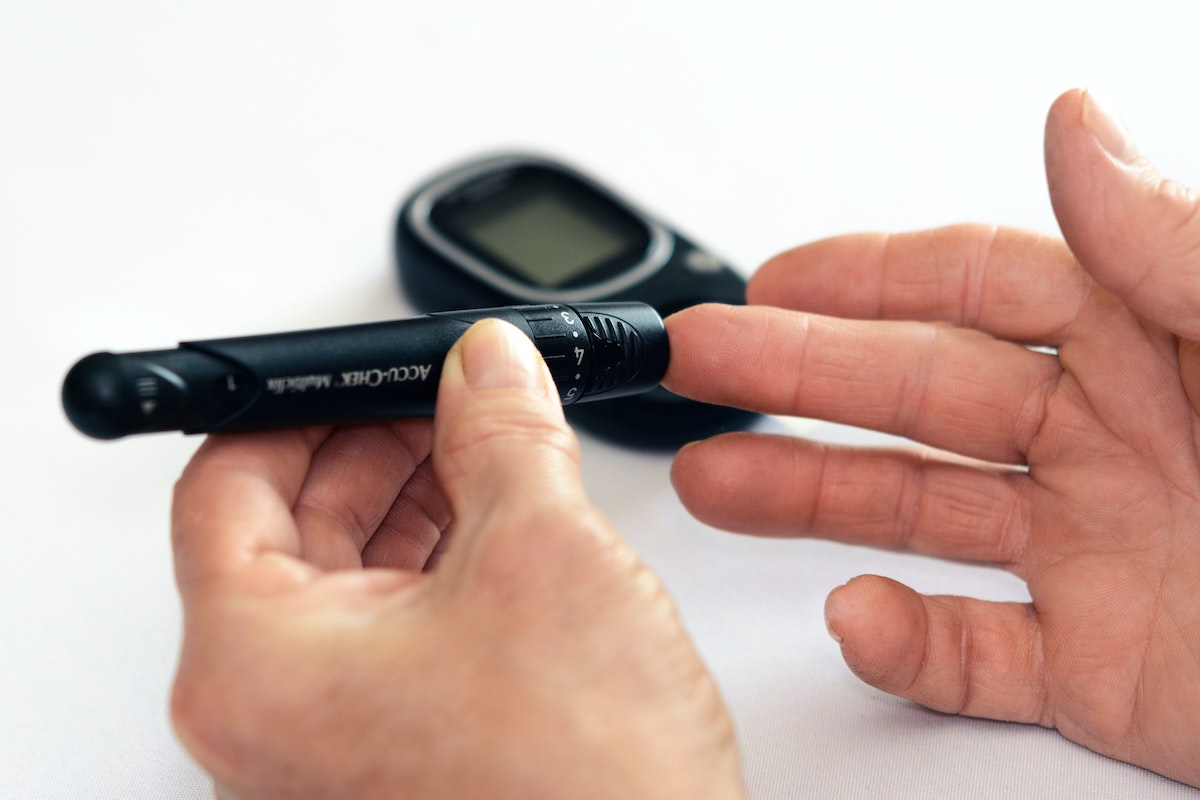
You may be diagnosed with gestational diabetes — or have type 2
Though the 1-hour test isn’t diagnostic, if your blood glucose levels exceed 200, it may be a sign you had diabetes before pregnancy. You’ll need to take another test 6 to 12 weeks postpartum to determine that.
In the meantime, if those blood glucose levels are high, your provider may recommend you skip further testing and proceed to gestational diabetes management. This management will likely include:
- Meeting with a dietician to discuss dietary tweaks to manage blood sugar
- Education and recommendation to increase exercise
- Checking blood sugar levels at home
- Extra monitoring through bloodwork and scans to ensure you and the baby are healthy
A word about the glucose test and gestational diabetes
Parenting guilt is real during pregnancy and after. Hearing that you “failed” a test can send you spiraling. It’s essential to remember that gestational diabetes is a hormonal reaction to pregnancy. You didn’t “cause it,” and you can’t “prepare” for it like a biology test. If you do wind up with gestational diabetes, your care team should give you all the tools you need in a non-judgmental way to manage symptoms and perhaps learn new ways to help your body thrive.